Quick Answer : Phantom Bite Syndrome (Occlusal Dysesthesia) is a neurological condition where a patient feels their bite is “wrong” despite no physical abnormality. It is caused by the brain becoming hyper-aware of tooth contact, often after a dental procedure. The best treatment is “Information Therapy,” stress management, and occasionally low-dose nerve-calming medications, rather than more dental adjustments.
Have you ever left a dental appointment feeling like your teeth don’t fit right anymore? You might have gone in for a simple filling or a new crown, but now, every time you close your mouth, something feels “high” or “off.” You go back for an adjustment, and your dentist tells you that, according to the marking paper, your bite is clinically perfect. Yet, the discomfort persists.
If you feel like you are being gaslit by your own jaw, you aren’t alone. This frustrating experience is often a sign of a real, documented condition known as Occlusal Dysesthesia (OD), or more commonly, Phantom Bite Syndrome (PBS) .
The Phantom in Your Jaw: Why Your Bite Feels Wrong After Dental Work
It is a common story in dental forums: a patient spends thousands on “dental shopping,” visiting specialist after specialist to find out why does my bite feel uneven. Most dentists are trained to look at the “hardware”—the teeth and the joints. But in Phantom Bite Syndrome, the problem isn’t the hardware; it’s the “software” in your brain .
What is Occlusal Dysesthesia (Phantom Bite Syndrome)?
Occlusal Dysesthesia is a persistent sensation (typically lasting more than 6 months) that your dental bite is wrong, even when there is no physical evidence of an abnormality in your teeth, gums, or jaw joints . A study published by Pelivan et al. in the Dental Journal (Basel) defines occlusal dysesthesia as “a challenging clinical entity characterized by persistent complaints of an uncomfortable, altered, or “wrong” bite sensation in the absence of objectively verifiable occlusal discrepancies”. The term “phantom” is used because the sensation of a “bad bite” exists even though the physical cause has been resolved or was never there to begin with .
The Science of “Occlusal Hyperawareness”: Why You Can’t Stop Thinking About Your Teeth
Under normal circumstances, your bite is a subconscious background process. Just like you don’t constantly feel the socks on your feet, you shouldn’t constantly feel your teeth touching. However, a routine procedure—like a bite feels off after filling—can act as a trigger. For most people, the brain adapts. For others with an uneven bite, the brain enters a state of “occlusal hyperawareness,” where it becomes impossible to ignore the sensation of the teeth meeting .
From Mechanics to Neurology: Why Your Brain is “Lying” to You
To understand why your bite feels high after crown work despite your dentist’s reassurance, we have to look at the connection between your mouth and your mind.
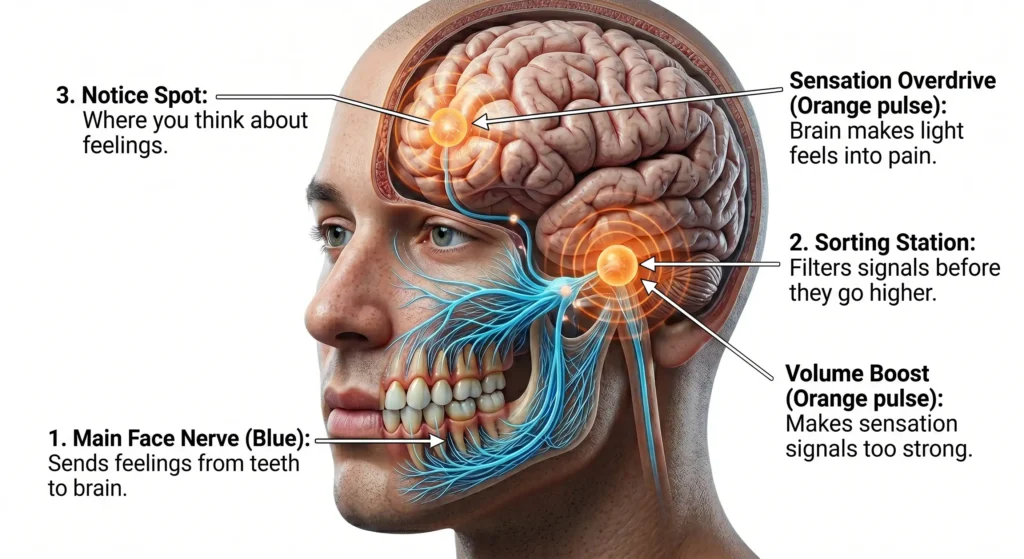
The Trigeminal Nerve and the Sensory “Volume Control” Knob
The trigeminal nerve is the massive communication highway between your teeth and your brain. It is packed with mechanoreceptors that are sensitive enough to detect a hair between your teeth . In Phantom Bite Syndrome, the “volume knob” on these sensory signals gets stuck at the maximum setting. This is known as maladaptive signal processing . Your brain is receiving accurate data that the teeth are touching, but it is interpreting that touch as “wrong” or “unpleasant” .
Why More Drilling and Adjustments Usually Make It Worse
One of the biggest dangers of PBS is the temptation to “fix” it with more dentistry. Another large-scale study of 199 patients observed that 155 of them (77.8%) had their symptoms triggered by dental treatments such as restorations, extractions, or orthodontics (Shinohara et al., 2019). When a dentist performs repeated adjustments or replaces crowns to satisfy a patient’s request, they are actually providing the brain with more new sensations to obsess over. This often entrenches the neurological “glitch” further .
Identifying the Symptoms: Is Your Bite Issue “Phantom”?
How do you know if your discomfort is a mechanical issue or Occlusal Dysesthesia? Clinical data shows that PBS typically follows a specific pattern.
- The Demographics: The condition predominantly affects middle-aged women, with the average age of onset around 50 to 53 years .
- The Duration: Symptoms often persist for years, with a mean duration of over 6 years reported in some studies .
- The “Dental Shopping” Cycle: Patients often visit an average of 4 to 5 different clinics seeking relief .
The Obsessive Checking Cycle: Tapping, Clenching, and Searching for Your Bite
A hallmark of PBS is the “checking” behavior. Patients may spend hours a day tapping their teeth together, looking in the mirror, or clenching their jaw to “find” the spot that feels wrong . This constant engagement keeps the brain’s sensory pathways on high alert, preventing the nervous system from ever “forgetting” the sensation.
The Hidden Link Between Stress, Anxiety, and Your Jaw
PBS is frequently associated with high-stress life phases or underlying anxiety and depression . Stress acts as an amplifier for sensory signals. If you are already in a state of high tension, your brain is more likely to hyper-fixate on a minor change in your mouth, leading to occlusal hyperawareness .
A Roadmap to Relief: How to Heal Without More Dental Work
The most important takeaway for anyone asking how to fix phantom bite syndrome without surgery is this: the answer is usually less dentistry, not more.
Information Therapy: Retraining Your Brain to Ignore the Bite
The first step in recovery is “Information Therapy.” This involves a thorough examination where your dentist uses objective tools—like T-Scan digital analysis or detailed marking paper—to show you that your teeth are, in fact, meeting correctly. Once you understand that the sensation is a neurological “phantom” and not a physical “fault,” you can begin the process of “defocusing”—consciously choosing to stop checking your bite .
The Role of Specialized Medications and Therapy in Finding Comfort
Because PBS is a disorder of signal processing, treatments that target the nervous system are often the most effective.
- Medications: Low-dose antidepressants like Amitriptyline or Milnacipran have shown significant success (up to a 55% reduction in discomfort) by “resetting” the sensory thresholds in the brain .
- Cognitive Behavioral Therapy (CBT): CBT helps patients manage the distress associated with the sensation and breaks the “obsessive checking” cycle .
- Stress Management: Techniques like mindfulness and biofeedback can help lower the overall “noise” in your nervous system, allowing the bite sensation to fade into the background .
- Bite Alignment Treatment: Visit your dentist for bite alignment treatment.
FAQ: Common Questions About Phantom Bite Syndrome
Q: Can a single high filling cause permanent bite issues? A: A high filling is a physical issue, but if it triggers occlusal hyperawareness, the sensation of a wrong bite can remain even after the filling is fixed .
Q: Why do my teeth feel even in the morning but wrong at night? A: This is often due to daytime stress and clenching. As you fatigue or experience stress during the day, your focus on your bite increases, making tiny, normal sensations feel significantly larger by the evening .
Q: What kind of doctor treats Phantom Bite Syndrome? A: You should look for an Orofacial Pain Specialist or a restorative dentist familiar with Occlusal Dysesthesia. Avoid any practitioner who promises a “quick mechanical fix” by grinding your teeth down .
Q: Are there medications for Phantom Bite? A: Yes. Certain medications that modulate nerve signals, such as tricyclic antidepressants (Amitriptyline), can be very effective at reducing the intensity of the sensation .

